
GUIDELINES
MANAGEMENT OF MAJOR DEPRESSIVE DISORDER (MDD)
CH Lim, B Baizury, on behalf of Development Group Clinical Practice Guidelines Management of Major Depressive Disorder
A. Introduction
Major depressive disorder (MDD) is a significant mental health problem that disrupts a person’s mood and affects his psychosocial and occupational functioning. It is often under-recognised and 30-50% of MDD cases in primary care and medical settings are not detected. Suicide occurs in up to 15% of hospitalised patients with severe MDD.
B. Screening
The routine use of screening instruments to identify depression is not recommended. However, the following two initial questions may be used to screen for depression:
- “During the past month, have you often been bothered by feeling down, depressed or hopeless?”
- “During the past month, have you often been bothered by having little interest or pleasure in doing things?”
If the answer is “Yes” to one or both questions, assess the patient for depression.
For this Two-Question Case-Finding Instrument, the reported sensitivity is 96% and specificity 57%, at a prevalence rate of 18%. Clinicians are encouraged to screen for at least these two core symptoms of depression, especially in high risk groups e.g. those with physical health problems causing disability, a past history of depression, a family history of depression and those with other mental health problems such as substance abuse or dementia.
C. Diagnosis
The diagnosis of MDD is made using internationally accepted diagnostic criteria i.e. either the 10th Revision of the International Classification of Diseases (refer Table 1) or the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders IV.
Table 1: ICD-10 diagnostic guidelines for depressive episode/depressive disorder:
Typical symptoms of depressive episodes: |
Common symptoms of depressive episodes: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Mild depressive episode: |
|
|
|
|
|
Moderate depressive episode: |
|
|
|
|
|
Severe depressive episode without psychotic symptoms: |
|
|
|
|
|
Adapted: WHO. ICD-10 Classification of Mental and Behavioural Disorders: Clinical Descriptions and Diagnostic Guidelines. Geneva: WHO: 1992
D. Referral
In the local setting, referral to the psychiatric services may be done through the Accident & Emergency Department or directly to the psychiatric clinic. There are circumstances where outpatient care may be insufficient and admission required. Locally, admission to the psychiatric unit can be voluntary or involuntary. Refer to Table 2 for Criteria for Referral and Admission.
Table 2: Criteria for referral and admission
Criteria for referral to psychiatric services: |
Criteria for admission: |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
E. Treatment
Management of MDD includes non-pharmacological with/without pharmacological measures depending on the severity of the disorder as shown in the Algorithm 1.Algorithm 1: Management of MDD
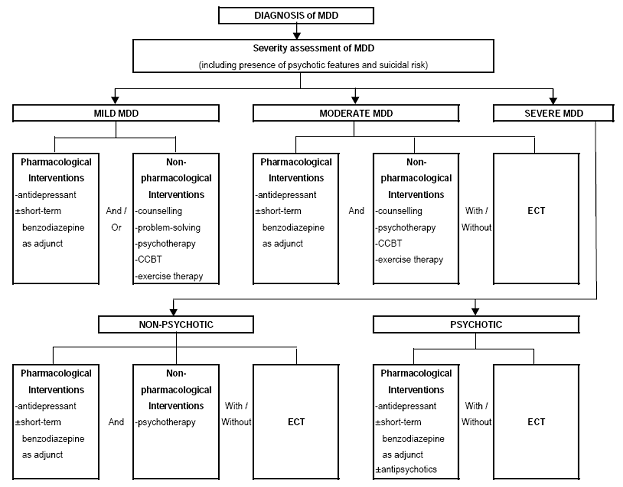
i. Mild major depressive disorder
A substantial proportion of primary care patients have mild major depressive disorder. There is more evidence for the effectiveness of antidepressants in moderate to severe depression than in mild depression (refer to Table 3 and Algorithm 2). Evidence supports the use of psychological interventions in the management of MDD.
Table 3: Treatment for mild MDD
Non-pharmacological interventions should be given. The patient should be followed up closely with a follow-up appointment within 2 weeks |
|
i. Psychological interventions:- |
|
|
|
|
|
|
|
ii. Other therapy such as exercise therapy |
|
Pharmacotherapy – SSRIs should be considered as the first line if medication is indicated |
|
ii. Moderate to severe major depressive disorder
NICE found that antidepressants are efficacious for reducing depressive symptoms and that SSRIs do not differ in efficacy from tricyclic antidepressants (TCAs) or monoamine oxidase inhibitors (MAOIs) in both in-patients and psychiatric outpatients or primary care patients. However, SSRIs are better tolerated compared to other antidepressants, and therefore, make appropriate drugs of first choice. Antidepressants are as effective as psychological interventions and more easily available in this country. Therefore, it is appropriate to offer them as a first-line measure. Refer to Table 4 and Algorithm 2 for Treatment for Moderate to Severe Major Depressive Disorder.
NICE also found some evidence favouring a combination of CBT plus antidepressants over antidepressants alone but there was insufficient evidence to say if this benefit persisted beyond the first few months. ECT is found to be superior to certain antidepressants in the short term but its effects are short-lived.Table 4: Treatment for moderate to severe MDD
Pharmacotherapy – SSRIs should be considered as the first line |
|
Non-pharmacological therapy |
|
i. Psychological interventions such as ognitive behavioural therapy (CBT) |
|
ii. Other therapy: |
|
|
|
iii. The role of Benzodiazepines
Benzodiazepines are not thought to have a specific antidepressant effect, and many experts believe that the depressive state is not improved by benzodiazepines alone. Clinicians may consider prescribing benzodiazepines as an adjunct to antidepressants. Avoid giving them alone, and as far as possible they should not be given for more than two to four weeks. Refer to Algorithm 1.
Commonly used antidepressants their dosages and adverse effects are shown in Table 5.
Table 5: Suggested antidepressant dosages and adverse effects
Name |
Starting dose* (mg/day) |
Usual dose (mg/day) |
Main adverse effects |
|---|---|---|---|
Selective Serotonin Reuptake Inhibitors (SSRIs) |
|||
Escitalopram |
10 |
10-20 |
Nausea, vomiting, dyspepsia, abdominal pain, diarrhoea, rash, sweating, agitation, anxiety, headache, insomnia, tremor, sexual dysfunction (male & female), hyponatraemia, cutaneous bleeding disorder. |
Sertraline |
50 |
50-200 |
|
Fluoxetine |
20 |
20 |
|
Fluvoxamine |
50-100 |
100-200 |
|
Tricyclics and tetracyclics |
|||
Amitriptyline |
25-75 |
75-200 |
Sedation, often with hangover, postural hypotension, tachycardia/arrhythmia, dry mouth, blurred vision, constipation, urinary retention. |
Clomipramine |
10-75 |
75150 |
|
Dothiepin |
50-75 |
75-225 |
|
Imipramine |
25-75 |
75-200 |
|
Maprotiline |
25-75 |
75-150 |
|
Reversible Inhibitor of MAO-I (RIMA) |
|||
Moclobemide |
150 |
150-600 |
Sleep disturbances, nausea, agitation, confusion. |
Serotonin and Noradrenaline Reuptake Inhibitor (SNRIs) |
|||
Venlafaxine, extended |
37.5-7.5 |
75-225 |
Nausea, insomnia, dry mouth, somnolence, dizziness, sweating, nervousness, headache, sexual dysfunction. |
Duloxetine |
40-60 |
60 |
|
Noradrenergic and Specific Serotonergic Antidepressant (NaSSA) |
|||
Mirtazapine |
15 |
15-45 |
Increased appetite, weight gain, drowsiness, oedema, dizziness, headache, blood dyscrasia. |
*Lower starting doses are recommended for elderly patients and for patients with significant anxiety, hepatic disease, or medical co-morbidity.
Algorithm 2: Pharmacotherapy of MDD

Details of the evidence supporting these recommendations can be found in the CPG on Management of MDD, available on the following websites: Ministry of Health Malaysia: http://www.moh.gov.my and Academy of Medicine: http://www.acadmed.org.my. Corresponding organization: CPG Secretariat, Health Technology Assessment Section, Medical Development Division, Ministry of Health Malaysia & contactable at htamalaysia@moh.gov.my
